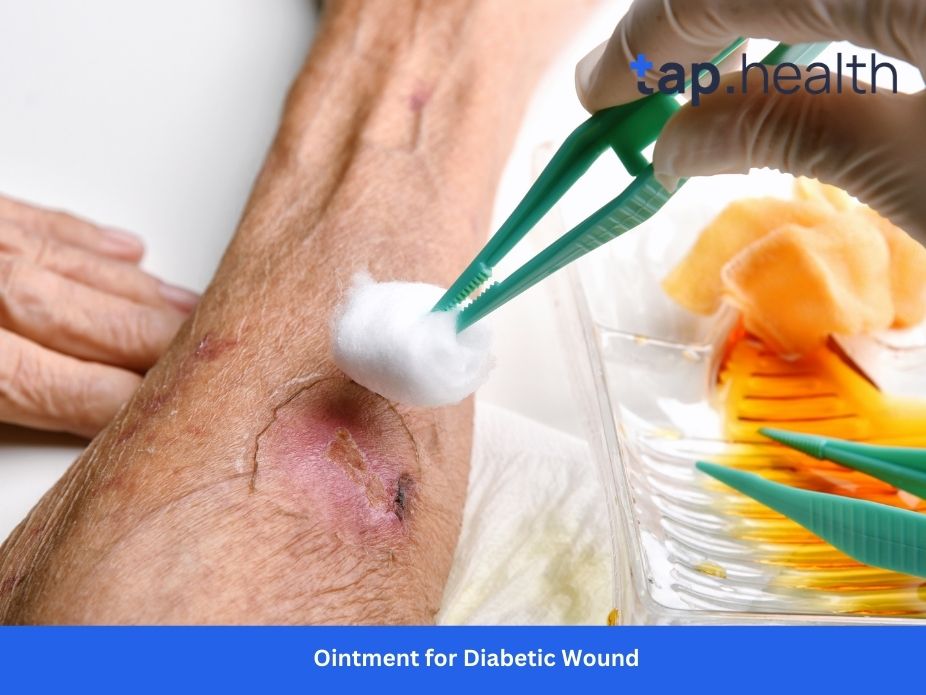
Living with diabetes means that a tiny scratch, a new shoe blister, or a small paper cut on your toe is never “just a scratch.” What takes three days to heal on a healthy person can quickly escalate into a massive, months-long medical crisis for someone with diabetes.
When you notice a break in your skin, your first instinct is likely to reach into your medicine cabinet, grab a tube of cream, and slather an ointment for diabetic wounds over the area. It seems like the logical, simple solution.
But in the world of diabetes, simple solutions can sometimes be the most dangerous.
Are over-the-counter antibiotic ointments safe for you? Can a simple cream heal a diabetic foot ulcer? When is putting an ointment on a wound actually making the infection worse?
In this highly detailed guide, we will break down exactly how to handle skin injuries when you have diabetes. We will explore the best ointments for minor cuts, the products you must strictly avoid, and the critical warning signs that tell you it is time to drop the tube of cream and rush to a doctor.
Is an Ointment Enough for a Diabetic Wound?
No, an ointment is rarely enough on its own. For a very minor, superficial scratch or a tiny cut that barely breaks the surface of the skin, a thin layer of a basic over-the-counter antibiotic ointment (like Neosporin or Soframycin) can be used as temporary first aid to keep the area clean.
However, if you are dealing with a diabetic foot ulcer—a deep, open sore—an ointment is absolutely not enough. In fact, smearing thick ointments into deep wounds can trap bacteria inside and cause the surrounding skin to become overly soggy and break down further. True diabetic wound care requires pressure relief (offloading), dead tissue removal, and specialised medical dressings, not just a cream.
Why Diabetic Wounds Need Extra Care
To understand why you cannot just rub an ointment on a cut and forget about it, you need to understand how diabetes changes your body’s plumbing and wiring.
Poor Blood Flow (Ischaemia): High blood sugar damages the blood vessels, particularly in your legs and feet. When a wound happens, your body needs to send oxygen-rich blood and white blood cells to the area to rebuild the skin and fight bacteria. If the blood vessels are narrow and stiff, the repair crew simply cannot reach the wound. Slower healing means the wound stays open longer.
Nerve Damage (Neuropathy): Diabetes destroys the nerves that feel pain. You might step on a nail or get a severe blister from a tight shoe and never feel it. Because you don’t feel it, you keep walking on it, driving the wound deeper into the flesh.
Higher Infection Risk: Bacteria love sugar. If your blood sugar is high, your tissues are saturated with glucose, providing a buffet for bacteria. If a diabetic wound is ignored, the infection can quickly reach the bone (osteomyelitis), leading to a massive amputation risk.
What Counts as a Diabetic Wound?
Not every injury is an ulcer. Knowing what you are dealing with helps you decide the treatment.
- Small Cut or Scratch: A minor, surface-level scrape.
- Blister: A fluid-filled bubble caused by friction from shoes.
- Cracked Heel: Deep fissures in dry skin that can split open and bleed.
- Callus-Related Wound: A thick buildup of hard skin that breaks down underneath, forming a hidden sore.
- Diabetic Foot Ulcer: A deep, crater-like open sore, usually on the bottom of the foot or the toes.
- Infected Wound: Any of the above that has become red, hot, swollen, or is leaking pus.
Can You Use Ointment on a Diabetic Wound?
The answer is a very cautious “sometimes.”
You may use a basic antibiotic ointment as a first-aid measure on small, cleaned, superficial wounds (like a paper cut on your finger or a minor scrape on your knee). The ointment creates a moist barrier that stops environmental bacteria from entering the fresh cut.
However, not all diabetic wounds should be self-treated. If the wound is on your foot, is deeper than the top layer of skin, or has been open for more than 48 hours without showing signs of closing, you must stop self-medicating. Deep ulcers need professional medical evaluation. Filling a deep hole with thick ointment prevents the doctor from seeing the true condition of the tissue and can trap anaerobic bacteria (bacteria that thrive without oxygen) deep inside the foot.
Types of Ointments Used for Diabetic Wounds
If a doctor advises topical treatment, they will recommend specific categories based on the wound’s exact needs.
Antibiotic Ointment for Minor Wounds
Over-the-counter ointments containing Bacitracin, Neomycin, or Polymyxin B (like Neosporin) or Framycetin (like Soframycin) are used strictly for very superficial cuts to prevent surface infection.
Prescription Topical Agents
If a wound has a specific bacterial load, a doctor might prescribe Mupirocin or a silver-based cream (like Silver Sulfadiazine) to actively kill the bacteria on the wound bed.
Moisture-Barrier Products
For extremely dry, cracked heels that have not yet bled, heavy moisturizing ointments containing urea or petroleum jelly are used to soften the skin and prevent it from splitting open.
Dressings vs Ointments
In modern diabetic clinics, ointments are rarely the main treatment for ulcers. Doctors prefer advanced dressings (like hydrogels, alginates, or foam dressings) that absorb excess fluid while keeping the wound perfectly moist, without leaving a greasy, messy residue behind.
Best Ointment for a Minor Diabetic Cut or Scratch
If you get a minor, shallow scratch on your arm or leg, here is the safest protocol to follow at home:
- Cleaning First: Wash the cut gently with mild soap and lukewarm running water. Do not scrub.
- Apply a Thin Layer: Use a clean cotton swab to apply a very thin, almost invisible layer of a basic antibiotic ointment (like Soframycin).
- Covering: Cover the scratch with a sterile, breathable adhesive bandage (Band-Aid).
- Daily Checking: Remove the bandage daily, wash the area, and check for any redness or swelling before reapplying a fresh bandage.
Ointment for Diabetic Foot Ulcer – Why It’s Not Just About Creams
If you have a diabetic foot ulcer (a deep sore on your foot), throwing an ointment on it is like putting a band-aid on a broken water pipe. It will not solve the underlying problem.
Healing a foot ulcer requires a massive, coordinated medical effort:
- Offloading: You must take 100% of your body weight off the wound using special boots or casts. No ointment will work if you keep walking on the sore.
- Debridement: A doctor must use a scalpel to physically cut away the dead, yellow, or black tissue inside the wound so fresh, healthy tissue can grow.
- Infection Control: This usually requires strong oral or IV antibiotics, not just a surface cream.
- Vascular Assessment: A surgeon must check if you actually have enough blood flow to heal the wound.
- Specialist Care: Deep ulcers require treatment by a podiatrist or a diabetic foot specialist.
When Antibiotic Ointment May Help
It is safe and helpful to use a simple antibiotic ointment ONLY when:
- It is a superficial minor wound (like a grazed knee).
- There is no deep tissue involvement (you cannot see fat or white tissue).
- There is no spreading infection (no redness travelling up your leg).
- You are using it as short-term home first aid (for 24 to 48 hours) while waiting to see if it heals or before your doctor’s appointment.
When Antibiotic Ointment Is Not Enough
You must stop using ointments and seek immediate medical help if you see any of these signs:
- The wound is a deep hole or ulcer.
- There is pus (yellow, green, or thick white discharge).
- The wound emits a bad, foul smell.
- There is redness spreading away from the wound into the surrounding skin.
- You have a fever or chills.
- There is black, dead tissue (eschar or gangrene) inside or around the wound.
- You experience severe pain, or conversely, if the wound is massive but you feel absolutely no pain (severe neuropathy).
- The wound is not healing after 3 or 4 days.
Ointments and Topical Products to Avoid in Diabetic Foot Ulcers
The pharmacy shelves are full of products that can actually destroy a diabetic foot. Avoid these completely:
- Herbal Wound Products / Unproven Remedies: Do not apply random pastes made of turmeric, neem, or unknown Ayurvedic powders into an open ulcer. These are not sterile and can introduce aggressive soil bacteria into the wound.
- Harsh Antiseptics: Never pour Hydrogen Peroxide, rubbing alcohol, Betadine, or Dettol directly into a deep diabetic ulcer. While they kill bacteria, they also violently kill the fragile new skin cells trying to heal the wound, severely delaying recovery.
- Over-the-Counter Steroid Creams: Creams containing hydrocortisone lower the local immune response and can cause a minor infection to explode out of control.
How to Clean a Diabetic Wound Before Applying Ointment
Proper hygiene is more important than the ointment itself.
- Wash Hands: Always wash your hands thoroughly with soap and water before touching your skin.
- Rinse Wound: Rinse the wound gently with clean, flowing drinking water or sterile saline solution. Do not soak the foot in a basin, as this spreads bacteria.
- Clean Surrounding Skin: Gently wash the intact skin around the wound, but do not scrub the open sore.
- Pat Dry: Use a clean, sterile gauze pad to pat the area completely dry. Never use a dirty bathroom towel.
- Apply Ointment: If appropriate, apply a paper-thin layer of ointment using a sterile Q-tip.
- Bandage Correctly: Cover it with a sterile, non-stick dressing and secure it with medical tape. Do not wrap the tape so tightly that it cuts off blood circulation.
How Often to Apply Ointment on a Diabetic Wound
- Follow Instructions: Always follow the specific instructions on the product or your doctor’s advice.
- Don’t Overapply: A massive, thick glob of ointment turns the skin white, soggy, and weak (maceration), making it easier for the wound to expand. Less is more.
- Change Dressing Regularly: Most minor wounds require a dressing change and a fresh, thin application of ointment once a day.
- Monitor Daily: Every time you change the dressing, look closely for any signs of worsening infection.
Ointment vs Dressing for a Diabetic Wound
Why do diabetic foot clinics rarely hand you a tube of cream? Because modern dressings are far superior.
Ointments are greasy. They melt, slide off the wound, and ruin your socks. They also do not absorb any of the fluid leaking from the wound.
Advanced medical dressings do multiple jobs at once. They manage exudate control (soaking up excess pus and fluid so the skin doesn’t get soggy). They provide physical cushioning for comfort. They maintain the perfect, slightly moist wound environment needed for skin cells to migrate and heal. Depending on the wound, your doctor might use a silver-infused foam dressing that continuously kills bacteria for three days without needing any messy ointments.
Signs a Diabetic Wound Is Infected
Because your immune system is compromised, infections move blindingly fast. Look for these undeniable signs:
- Redness: A bright red halo around the wound that expands daily.
- Warmth: The skin around the wound feels noticeably hotter to the touch than the rest of your leg.
- Swelling: The foot or toe becomes puffy and tight.
- Drainage: Leaking thick, cloudy, yellow, or green fluid (pus).
- Foul Smell: A rotting or sweet, sickly odour coming from the bandage.
- Delayed Healing: A wound that has not changed size or has gotten bigger after a week.
- Deeper Tissue Concern: You can see white bone or shiny yellow tendons at the bottom of the hole.
When a Diabetic Wound Needs Oral Antibiotics or Hospital Care
Topical ointments only treat the very surface of the skin. If bacteria have invaded the deep tissues, you need systemic help.
If the redness is spreading up your leg (cellulitis), if there is a deep infection, or if the doctor suspects the infection has reached the bone (osteomyelitis), you will urgently need strong oral antibiotics or intravenous (IV) antibiotics in a hospital.
If the wound is accompanied by systemic symptoms like a high fever, a racing heart, or extreme confusion, the infection has entered your bloodstream (sepsis). If your toes turn black and cold (gangrene) due to poor circulation, emergency surgery is required to save the limb.
Best Treatment Plan for a Diabetic Foot Wound (Beyond Ointment)
Healing a diabetic ulcer is a team effort. Here is what a proper medical protocol looks like:
- Blood Sugar Control: Healing stops completely if your blood sugar is high. You must bring your HbA1c and daily numbers into the target range immediately.
- Offloading: Using special crutches, wheelchairs, or cast boots to ensure zero pressure touches the wound.
- Debridement: The doctor physically cleans out the dead tissue.
- Infection Treatment: Using the correct oral antibiotics based on a wound swab culture.
- Dressing Selection: Applying advanced, moisture-balancing medical dressings.
- Circulation Check: Ensuring you have enough blood flow to the foot, sometimes requiring vascular surgery to open blocked arteries.
- Team-Based Care: Working with an endocrinologist, a podiatrist, and a wound care nurse simultaneously.
How Blood Sugar Control Affects Wound Healing
You can apply the most expensive ointment in the world, but if your blood sugar is 250 mg/dL, the wound will not close.
High blood sugar thickens the blood and narrows the vessels, causing poor circulation. It paralyzes your white blood cells, making them slow and weak, drastically increasing your infection risk. It also prevents the production of collagen, which is the essential building block needed to weave new skin together. Controlling your glucose is the ultimate wound-healing “ointment.”
Home Care Tips for a Small Diabetic Wound
If you get a minor scratch, be proactive:
- Daily Inspection: Check your feet every single night using a mirror to spot tiny cuts before they become big ulcers.
- Clean Dressing: Keep the minor wound covered and clean at all times.
- Avoid Walking Barefoot: Never walk barefoot, even inside your own house, to prevent stepping on unseen sharp objects.
- Don’t Pop Blisters: If your shoe causes a blister, leave it alone. Popping it creates an open door for massive infection.
- Protect Pressure Areas: Wear soft, seamless, diabetic-friendly socks and well-fitting shoes.
Real-Life Scenario
Mr. Gupta, a 60-year-old with Type 2 diabetes, noticed a small blister on the side of his big toe after wearing new shoes. Because of his neuropathy, it didn’t hurt. He popped the blister with a needle, rubbed some herbal turmeric paste into it, and covered it with a tight bandage.
Three days later, he felt feverish. When he took off the bandage, his entire toe was swollen, bright red, and leaking foul-smelling pus. The herbal paste had trapped soil bacteria inside the open wound.
His son rushed him to a diabetic foot clinic. The doctor had to surgically cut away the dead, infected tissue (debridement) and start Mr. Gupta on strong IV antibiotics to stop the infection from reaching the bone. The doctor explained that putting unsterile pastes or thick ointments into an open diabetic wound is highly dangerous. Mr. Gupta learned that a diabetic foot wound requires sterile dressings, offloading, and immediate professional medical care, not bathroom-cabinet remedies.
Expert Contribution
We asked Dr. Rajan Sharma, a leading Podiatric Surgeon specialising in diabetic limb salvage, about the misuse of ointments:
“The biggest frustration in my clinic is when a patient arrives with a deep foot ulcer completely packed with a thick layer of over-the-counter antibiotic ointment.
Patients think they are helping, but they are actually suffocating the wound. Deep ulcers need to breathe and drain. When you plug the hole with a greasy ointment, the infected fluid backs up into the foot, destroying healthy tissue. I always tell my patients: if it is a tiny surface scratch, a thin dab of Neosporin is fine. But if it is a deep hole on the bottom of your foot, do not put anything in it. Cover it with a dry, sterile gauze pad and come to the clinic immediately. Time is tissue.”
Recommendations Grounded in Proven Research and Facts
The medical protocol for diabetic wound care is strict and heavily researched.
According to the International Working Group on the Diabetic Foot (IWGDF), there is no robust clinical evidence to support the routine use of topical antimicrobial ointments for treating chronic diabetic foot ulcers. The primary standard of care dictates that ulcers must be managed through adequate offloading, sharp debridement, and the use of sterile, non-adherent dressings to maintain a moist (but not soggy) wound environment.
Furthermore, the American Diabetes Association (ADA) strongly advises against patients attempting to self-treat foot ulcers with over-the-counter antiseptics or ointments. The ADA emphasizes that any foot ulcer requires immediate evaluation by a healthcare professional to assess for deep-tissue infection and peripheral arterial disease.
Conclusion: Key Takeaways
So, what is the final verdict on using an ointment for diabetic wounds?
- For minor, shallow scratches: A very thin layer of basic antibiotic ointment (like Soframycin) is safe as temporary first aid.
- For deep foot ulcers: Do NOT use over-the-counter ointments. They trap bacteria and ruin the wound bed.
- Hygiene is critical: Wash wounds with clean water and pat dry. Never use harsh chemicals like Dettol or Hydrogen Peroxide on an open sore.
- Look for red flags: If the wound is red, hot, swollen, smells bad, or has pus, you need oral antibiotics from a doctor immediately.
- Treat the root cause: No ointment will work if you do not control your blood sugar and keep your body weight off the injured foot.
Treat every single break in your skin with extreme caution. When in doubt, always let a medical professional look at your foot.
Frequently Asked Questions on Ointment for Diabetic Wound
What is the best ointment for diabetic wounds?
There is no single “best” ointment, as it depends on the wound. For a very minor, superficial scratch, a basic antibiotic ointment like Neosporin, Bacitracin, or Soframycin is fine for first aid. However, for deep diabetic foot ulcers, doctors do not use over-the-counter ointments; they use advanced medical dressings and prescription topical agents.
Is Betadine or Dettol safe for diabetic wounds?
No. You should never pour harsh antiseptics like Betadine, Dettol, rubbing alcohol, or Hydrogen Peroxide directly into an open diabetic wound. While they kill bacteria, they are highly toxic to the fragile new skin cells trying to heal the wound, which severely delays the healing process.
Can I use a steroid cream on a diabetic foot ulcer?
Absolutely not. Over-the-counter steroid creams (like hydrocortisone) suppress the local immune system and reduce inflammation. If you put them on an open wound, you are turning off your body’s natural defense mechanism, allowing the bacteria to multiply wildly and turn a small infection into a massive one.
How do I know if my diabetic wound is infected?
Signs of a dangerous infection include spreading redness around the wound, the skin feeling hot to the touch, swelling, thick yellow or green pus, a foul odour, fever, or a wound that continues to get larger rather than smaller after a few days.
What should I do if my diabetic foot wound won’t heal?
If a wound on your foot has not shown significant improvement or closure after 3 to 4 days, or if it is a deep ulcer, you must visit a doctor or a specialized diabetic foot clinic immediately. Delayed healing usually indicates poor blood flow, an underlying bone infection, or uncontrolled blood sugar, all of which require professional medical intervention.
Disclaimer: This article is for informational and educational purposes only and does not constitute medical advice. A diabetic foot ulcer can lead to severe complications, including amputation. Always consult your doctor, podiatrist, or wound care specialist immediately for any skin injuries or non-healing wounds.