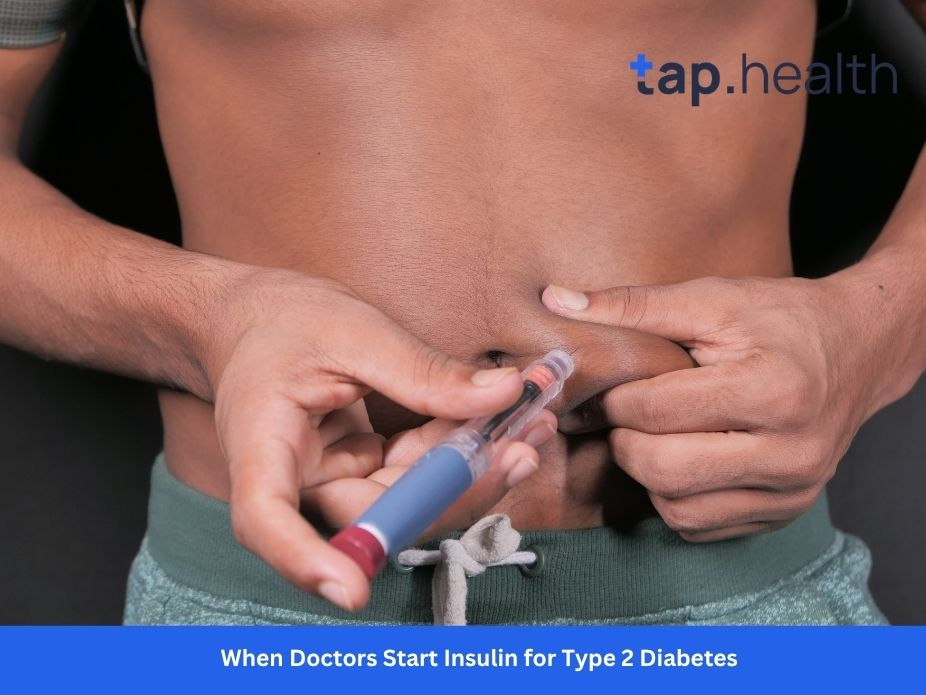
If you have been living with type 2 diabetes for some time, you have probably heard the word “insulin” whispered in your doctor’s office or mentioned by a worried family member. For many people, the thought of starting insulin can feel like a personal failure or a sign that their health is spiralling out of control. There is often a deep-seated fear that taking insulin means the disease has become “serious” or that life will become more complicated and restricted.
Let me start by telling you something very important: starting insulin is not a failure. It is not a punishment. It is simply a smart, logical, and often necessary next step in a long journey. Type 2 diabetes is a progressive condition, which means that over time, the pancreas—the organ that makes insulin—can get tired and produce less of this vital hormone. When that happens, the oral medications you have been relying on may no longer be enough to keep your blood sugar in a healthy range.
Understanding exactly when and why doctors recommend insulin can take away a lot of the fear and uncertainty. It empowers you to work with your healthcare team, rather than feeling like something is being done to you. This comprehensive guide will walk you through everything you need to know: the specific numbers your doctor looks for, the symptoms that signal a need for change, the different types of insulin available today, and what you can expect from life on insulin therapy. Our goal is to replace fear with clear, reliable knowledge.
Understanding the Progressive Nature of Type 2 Diabetes
To grasp why insulin eventually becomes necessary, you first need to understand the underlying story of type 2 diabetes. It is not a static condition; it changes over time.
The primary problem in type 2 diabetes is insulin resistance. This means that your body’s cells—particularly in your muscles and liver—do not respond properly to the insulin your pancreas produces. Imagine insulin as a key trying to unlock a door to let sugar (glucose) into your cells. With insulin resistance, the lock is rusty and the key doesn’t work very well.
To compensate, your pancreas works overtime, pumping out more and more insulin to try and force that door open. For many years, this can work. Your blood sugar may stay relatively normal, but at a huge cost: your pancreas is under constant, tremendous stress. Over time, the beta cells in the pancreas that produce insulin become exhausted and begin to fail. They produce less and less insulin. This is the progressive nature of type 2 diabetes.
This is why a person may manage their diabetes with diet and exercise alone for a few years, then need one oral medication, then two or three, and eventually, may require insulin. It is not because you did something wrong. It is the natural history of the disease. Starting insulin is a way to give your tired pancreas a rest and provide your body with the hormone it desperately needs to function correctly.
When Do Doctors Decide to Start Insulin? Key Scenarios
The decision to start insulin is not made lightly, but it is based on clear clinical evidence and well-established guidelines. Doctors look for specific signs and thresholds that indicate oral medications are no longer providing adequate control. The decision can happen in a few common scenarios.
Scenario 1: Oral Medications Are No Longer Enough (High HbA1c)
The most common path to starting insulin is when a person’s blood sugar remains too high despite taking multiple oral diabetes medications.
Your doctor uses a blood test called HbA1c (or A1c for short) to understand your average blood sugar levels over the previous two to three months. This is the single most important number for guiding long-term treatment decisions.
Major health organisations, including the American Diabetes Association (ADA) and the National Institute for Health and Care Excellence (NICE) in the UK, have set clear thresholds.
According to expert consensus and NICE guidelines, insulin therapy is generally indicated when other measures (like diet, exercise, and oral drugs) no longer achieve adequate blood glucose control, typically defined as an HbA1c target of less than 7.0% to 7.5%. If a person has been on two or three oral medications at maximum tolerated doses for 3 to 6 months and their HbA1c remains above this target, it is time to have a serious conversation about starting insulin.
At What Level of HbA1c is Insulin Started?
- HbA1c persistently >7.0% to 7.5% despite being on multiple oral drugs is a strong indication to consider initiating insulin therapy.
- HbA1c ≥ 9.0% (75 mmol/mol): If a person’s HbA1c is this high, especially if they are already on oral medications, guidelines recommend considering a combination of basal (long-acting) and short-acting insulin right from the start. This is because the body’s own insulin production is clearly inadequate.
- HbA1c ≥ 10%: At this level, particularly if the patient is already on multiple oral agents, the ADA guidelines recommend strongly considering insulin therapy without delay.
It is important to understand that these are guidelines, not rigid rules. Your doctor will personalise these targets based on your age, overall health, risk of low blood sugar (hypoglycaemia), and other medical conditions you may have.
Scenario 2: Immediate Need at Diagnosis (Very High Blood Sugar)
Sometimes, insulin is not a “later” option but a “right now” requirement. Some people are diagnosed with type 2 diabetes when their blood sugar is already dangerously high.
If a newly diagnosed person has an HbA1c of 9.0% or higher, or a fasting blood glucose (FPG) level of 11.1 mmol/L (200 mg/dL) or higher, and is experiencing significant symptoms of high blood sugar, doctors will often recommend short-term intensive insulin therapy.
This approach, sometimes called “insulin first,” can quickly bring blood sugar down to a safe level. Research shows that this short-term use of insulin can sometimes help “rest” the pancreas and restore some of its natural function, a concept known as “beta-cell rest.” After a period of weeks or months on insulin, some people are able to transition back to oral medications alone and maintain good control for a period of time.
Scenario 3: Severe Symptoms of Hyperglycaemia
Sometimes, the decision to start insulin is not based on a number from a lab test but on how a person is feeling. Severe, uncontrolled high blood sugar causes a set of unmistakable symptoms. If you are experiencing these, your doctor will likely start insulin immediately, regardless of your HbA1c.
These symptoms are a sign of metabolic decompensation and include:
- Polyuria: Urinating much more often than usual, especially waking up multiple times at night to go to the bathroom.
- Polydipsia: An unquenchable, intense thirst.
- Unintentional Weight Loss: Losing weight without trying, despite eating normally or even more than usual. This happens because your body cannot use the sugar in your blood for energy and starts breaking down muscle and fat for fuel instead.
- Blurred Vision: High blood sugar can cause the lens of your eye to swell, changing your vision.
- Fatigue and Weakness: Feeling constantly tired and run-down.
If a person presents with these symptoms, insulin is the fastest and most effective way to correct the problem and make them feel better.
Scenario 4: Acute Medical Events or Special Circumstances
There are several other situations where insulin may be needed, often for a temporary period:
- Acute Illness or Infection: When you are very sick (e.g., with a severe flu, pneumonia, or a serious infection), your body releases stress hormones that make your blood sugar skyrocket. Oral medications may not be able to control this surge, and a short course of insulin may be necessary to get you through the illness.
- Major Surgery: Around the time of a major operation, blood sugar control is critical for proper wound healing and preventing infections. Many people with type 2 diabetes who are on oral medications will be temporarily switched to insulin during their hospital stay and recovery period.
- Pregnancy: If you become pregnant and have type 2 diabetes, or if you develop gestational diabetes, insulin is the safest and most effective medication to manage blood sugar and protect the health of both the mother and the baby. Most oral diabetes medications are not recommended during pregnancy.
- Diabetic Ketoacidosis (DKA) or Hyperosmolar Hyperglycemic State (HHS): These are life-threatening emergencies caused by severe insulin deficiency. Their treatment requires immediate hospitalisation and intravenous (IV) insulin.
Which Insulin is Best for Type 2 Diabetes? A Clear Overview
If your doctor recommends insulin, the next question is: “What kind?” The world of insulin has changed dramatically in the last few decades. It is no longer just about one or two injections a day. There are now many different types of insulin, each designed to work in a specific way. The “best” insulin is the one that fits your lifestyle, your eating patterns, and your body’s needs.
Long-Acting Insulin (Basal Insulin): The Foundation of Treatment
For most people with type 2 diabetes who are starting insulin, the first step is a long-acting (basal) insulin. This type of insulin is designed to provide a slow, steady release of insulin over a 24-hour period. It acts as a “background” or “baseline” insulin, controlling your blood sugar between meals and while you sleep. It does not cover the sugar spikes that happen when you eat a meal.
Common Long-Acting Insulin Names:
- Insulin Glargine: Brand names include Lantus, Basaglar, Toujeo, Semglee, and Abasaglar.
- Insulin Detemir: Brand name is Levemir (Note: Levemir is being phased out globally, with supplies expected to last until late 2026 in some regions).
- Insulin Degludec: Brand name is Tresiba. This is an ultra-long-acting insulin that can last for more than 40 hours, offering more flexibility in the timing of your daily injection.
Most people starting long-acting insulin will take it once a day, usually at the same time each day (often at bedtime). The NICE guidelines recommend offering basal insulin as the initial insulin therapy for most adults with type 2 diabetes.
Rapid-Acting or Short-Acting Insulin (Prandial Insulin)
If your blood sugar is still too high after a meal despite taking a long-acting insulin, your doctor may add a rapid-acting (prandial) insulin. “Prandial” means “relating to a meal.” You take this type of insulin just before you eat to cover the carbohydrates in your meal and prevent a post-meal blood sugar spike.
Common Rapid-Acting Insulin Names:
- Insulin Lispro (Humalog)
- Insulin Aspart (NovoLog)
- Insulin Glulisine (Apidra)
This approach is often called a basal-bolus regimen. You take a long-acting insulin once or twice a day for your background needs, and a rapid-acting insulin with each meal. This provides the most precise control and most closely mimics how a healthy pancreas works.
Pre-Mixed Insulin (Biphasic Insulin): A Convenient Compromise
For some people, the simplicity of fewer injections is a priority. Pre-mixed (biphasic) insulin combines both a medium-acting and a rapid- or short-acting insulin in a single vial or pen. This means you get both a background insulin effect and a mealtime insulin effect from one injection.
These insulins are typically taken once or twice a day before meals. The main trade-off is less flexibility. Because the ratio of the two insulins is fixed, you must eat your meals at consistent times and with a consistent amount of carbohydrates each day to avoid low or high blood sugar. This is a good option for people with very regular routines and eating habits.
What is the Average Dose of Insulin for Type 2 Diabetes?
There is no “one-size-fits-all” dose for insulin. Your starting dose will be calculated based on your body weight and how sensitive you think you are to insulin. From there, the dose will be carefully adjusted over weeks and months.
How the Starting Dose is Calculated
A common method doctors use is to calculate the total daily insulin requirement as 0.1 to 0.5 units of insulin per kilogram of body weight. For people with type 2 diabetes, who often have significant insulin resistance, the requirement may be higher, in the range of 0.5 to 0.8 units per kg per day.
Example Calculation for Starting Basal Insulin:
- For a person weighing 80 kg, the starting dose might be calculated at 0.2 units/kg.
- This equals 80 kg × 0.2 units = 16 units of long-acting insulin per day.
This is often rounded to a number that is easy to measure on an insulin pen (e.g., 15 or 20 units). The doctor will then instruct you on how to slowly and safely increase this dose based on your morning blood sugar readings.
How the Dose is Adjusted: The “3-Day Rule”
Once you start insulin, the dose is not set in stone. You and your healthcare team will work together to “titrate,” or adjust, the dose until you reach your blood sugar targets.
This is where the “3-day rule” comes in. The core principle is that you should not change your insulin dose based on a single high or low reading, as blood sugar can fluctuate day-to-day. Instead, you look for a consistent pattern.
Guidelines recommend that insulin doses should be adjusted every three or four days until the target blood glucose levels are reached. Here is how it works in practice:
- Monitor Your Blood Sugar: You check your fasting blood sugar every morning for three days.
- Look for a Pattern: If your fasting blood sugar is above your target range for three days in a row, it is time to increase your long-acting insulin dose.
- Adjust the Dose: The ADA recommends increasing the dose by 2 units every 3 days if fasting glucose is between 140-179 mg/dL (7.8-9.9 mmol/L), or by 4 units every 3 days if it is 180 mg/dL (10.0 mmol/L) or higher.
- Repeat: You continue this cycle of monitoring and small adjustments until your fasting blood sugar is consistently in your target range.
This method is safe and effective, preventing large swings in blood sugar and reducing the risk of dangerous hypoglycaemia (low blood sugar).
Benefits and Side Effects of Insulin for Type 2 Diabetes
Like any powerful medical treatment, insulin has both clear benefits and potential side effects. It is essential to understand both sides to make an informed decision and manage your therapy well.
The Major Benefits
- Superior Blood Sugar Lowering: Insulin is the most potent and effective medicine available for lowering blood glucose. It can bring even very high blood sugar levels down quickly and safely.
- Prevention of Long-Term Complications: By achieving better blood sugar control, insulin helps prevent or delay the serious long-term complications of diabetes. This includes damage to the eyes (retinopathy), kidneys (nephropathy), nerves (neuropathy), and heart.
- Flexibility and Personalisation: With modern insulins and pens, you and your doctor can tailor a regimen that fits your unique life, allowing for greater flexibility in meal timing and activity.
- Symptom Relief: If you were experiencing symptoms of high blood sugar—like constant thirst, frequent urination, and fatigue—starting insulin will relieve these symptoms and help you feel much better, often within days.
The Main Side Effects and How to Manage Them
- Hypoglycemia (Low Blood Sugar): This is the most common and most serious potential side effect of insulin therapy. It happens when your blood sugar drops too low (usually below 70 mg/dL or 3.9 mmol/L). Symptoms include shakiness, sweating, confusion, and heart palpitations. Why it happens: Taking too much insulin, skipping a meal, or exercising more than usual. How to manage it: Always carry a fast-acting source of sugar (like glucose tablets, candy, or juice). Learn to recognise your own early warning signs. This is a primary reason why careful dose titration and education are so critical.
- Weight Gain: Insulin helps your body store sugar and fat more efficiently, which can lead to modest weight gain for some people. This effect can be minimised by pairing insulin with metformin (which has weight-neutral or weight-loss effects) and by being mindful of diet and exercise.
- Injection Site Reactions: You may experience some redness, swelling, or itching at the injection site. This is usually mild and goes away on its own. The key is to rotate your injection sites (e.g., abdomen, thigh, upper arm) to prevent the buildup of scar tissue or fatty lumps (lipohypertrophy), which can affect insulin absorption.
What About Non-Insulin Injectables Like Ozempic?
You may have heard about newer, non-insulin injectable medications like Ozempic, Wegovy, and Mounjaro (which are GLP-1 receptor agonists). These drugs are highly effective for lowering blood sugar and promoting weight loss.
In modern diabetes care, these medications are often used before insulin is started. They can help people achieve good blood sugar control for many more years, potentially delaying or even avoiding the need for insulin altogether. However, if these medications, combined with oral drugs, are no longer enough to control blood sugar, the next step is still often insulin.
Real-Life Scenario: From Fear to Freedom
Let’s look at a common situation to make this more relatable.
Meet Mr. Sharma.
Mr. Sharma is a 60-year-old retired bank manager from Jaipur. He was diagnosed with type 2 diabetes 12 years ago. For the first few years, he managed his condition well with metformin and regular evening walks. Over time, his HbA1c crept up, so his doctor added a second medication, glimepiride, and then a third, empagliflozin.
Despite taking all his pills faithfully, Mr. Sharma noticed he was always thirsty and waking up two or three times a night to use the bathroom. He felt tired all the time. His recent HbA1c came back at 8.8%. His doctor, Dr. Verma, gently suggested it was time to consider adding a small dose of insulin.
Mr. Sharma’s Initial Fear:
Mr. Sharma’s heart sank. He felt like he had failed. He remembered his uncle who had to take injections and was terrified of needles and the thought of his life being ruled by a strict schedule. He thought, “This is the beginning of the end.”
How Dr. Verma Addressed It:
Dr. Verma listened to his fears and explained things simply: “Mr. Sharma, your body has been fighting this for over a decade. Your pancreas is tired. This is not your fault. Adding a small amount of long-acting insulin once a day is like giving your pancreas a much-needed helper. It will take the pressure off and allow you to feel better.”
Dr. Verma explained the “3-day rule” for adjusting the dose and reassured him that with modern insulin pens, the needles are tiny and virtually painless. He started Mr. Sharma on just 12 units of long-acting insulin at bedtime.
The Outcome:
Mr. Sharma was nervous but gave it a try. To his surprise, the injection was barely a pinch. He started checking his fasting blood sugar each morning and adjusting his dose by 2 units every few days as instructed. Within two weeks, his morning readings were in a healthy range for the first time in years. The constant thirst and nighttime bathroom trips stopped. He had more energy and felt more like his old self.
Six months later, his HbA1c had dropped to 7.0%. He told Dr. Verma, “I was so scared of insulin, but it has given me my life back. I wish I had started sooner.”
Expert Contribution
To provide a clinical perspective, we can look to the consensus from major diabetes organisations.
“Insulin therapy should be considered for people with type 2 diabetes who have inadequate glycemic control on non-insulin therapies. The decision to initiate insulin should be based on an individualised assessment, taking into account the degree of hyperglycemia, the presence of symptoms, and the patient’s overall health status and preferences. A common practice is to initiate insulin when the HbA1c is above 7.0-7.5% despite optimal use of oral agents, or immediately if the HbA1c is 9.0% or higher with symptoms of hyperglycemia. The goal is to safely achieve and maintain glycemic targets while minimizing hypoglycemia and weight gain.”
This perspective, which aligns with guidelines from the ADA and NICE, reinforces that starting insulin is a thoughtful, evidence-based decision aimed at preserving long-term health and quality of life.
Recommendations Grounded in Proven Research and Facts
Based on a thorough review of current clinical guidelines and research, here are clear, actionable recommendations:
- Do Not Fear Insulin: Understand that starting insulin is a normal and expected part of the progression of type 2 diabetes for many people. It is a sign that your disease is changing, not that you have failed.
- Know Your Numbers: Track your HbA1c and have an open conversation with your doctor about what your personal target should be. If your numbers are consistently above target, ask about all your options, including insulin.
- Educate Yourself: If insulin is recommended, ask for a structured education programme. You should learn proper injection technique, how to self-monitor your blood sugar, how to adjust your dose, and how to prevent and treat hypoglycemia. Knowledge is your best defense against fear.
- Be an Active Participant: Work with your doctor to choose the insulin regimen (long-acting, mixed, or basal-bolus) that best fits your lifestyle and preferences.
- Follow the “3-Day Rule” for Titration: Do not make impulsive changes to your insulin dose based on a single reading. Look for consistent patterns over several days and make small, steady adjustments as guided by your healthcare team.
Key Takeaways
- The need for insulin in type 2 diabetes is a result of the progressive nature of the disease as the pancreas produces less insulin over time.
- Doctors typically start insulin when the HbA1c is persistently above 7.0-7.5% despite the use of multiple oral medications.
- Insulin may be started immediately at diagnosis if the HbA1c is 9.0% or higher, especially if symptoms of high blood sugar are present.
- The first insulin used is usually a long-acting (basal) insulin taken once daily.
- The dose is carefully adjusted using a safe, stepwise approach known as the “3-day rule.”
- While insulin can cause side effects like low blood sugar (hypoglycemia) and weight gain, these can be effectively managed with proper education and dose titration.
- Modern insulin pens and tiny needles make taking insulin a simple, relatively painless part of a daily routine that can dramatically improve your health and quality of life.
Frequently Asked Questions (FAQs) on When Doctors Start Insulin for Type 2 Diabetes?
Q1: At what HbA1c level do you start insulin for type 2 diabetes?
A: Insulin is typically considered when a person’s HbA1c remains above 7.0-7.5% despite being on two or three oral medications. For a newly diagnosed person with an HbA1c of 9.0% or higher and significant symptoms, doctors may start insulin immediately.
Q2: What is the “3-day rule” for insulin?
A: The “3-day rule” is a safe method for adjusting insulin doses. You monitor your blood sugar for three days, and if the levels are consistently above your target, you adjust your dose by a small amount (e.g., 2 units) every 3-4 days until you reach your goal. This prevents over-correction and reduces the risk of low blood sugar.
Q3: What is the best insulin for type 2 diabetes?
A: There is no single “best” insulin. For most people starting out, a long-acting (basal) insulin (like Lantus or Tresiba) taken once daily is the recommended first step. If more control is needed, a rapid-acting insulin before meals or a pre-mixed insulin may be added.
Q4: What are the main side effects of insulin for type 2 diabetes?
A: The most common and serious side effect is hypoglycemia (low blood sugar). Other potential side effects include weight gain and mild injection site reactions. These can be managed with proper education, dose adjustment, and site rotation.
Q5: What is the average starting dose of insulin for type 2 diabetes?
A: The starting dose is calculated based on your body weight. A common starting point for long-acting insulin is around 0.1 to 0.2 units of insulin per kilogram of body weight per day. For an 80 kg person, this would be around 10-16 units.
Q6: Does starting insulin mean my diabetes is getting worse?
A: It means your diabetes is progressing, which is a normal part of the disease for many people. It is not a sign of personal failure. It simply means your body needs more help to keep your blood sugar in a healthy range and prevent future complications.
Q7: Can I stop insulin once I start taking it?
A: In some cases, yes. If insulin is started for a short-term reason, like during a severe illness or surgery, you can often stop it afterwards. Some people who start insulin at diagnosis may also be able to transition back to oral medications. However, for many people with long-standing diabetes, insulin is a long-term therapy.
Q8: What is the difference between long-acting and rapid-acting insulin?
A: Long-acting (basal) insulin provides a slow, steady release of insulin over 24 hours to control blood sugar between meals and overnight. Rapid-acting (prandial) insulin is taken just before a meal and works quickly to manage the blood sugar spike from the food you eat.
References
- NICE. (2025). Type 2 diabetes in adults: management (NG28). https://www.nice.org.uk/guidance/ng28
- NHS. (2023). Insulin for type 2 diabetes. https://www.nhs.uk/medicines/insulin/insulin-for-type-2-diabetes/
- American Diabetes Association. (2025). Standards of Care in Diabetes—2025. https://diabetesjournals.org/care/issue/48/Supplement_1